All the Health Insurance Words You Need to Know But Were Too Embarrassed to Ask About – Lifehacker

Photo: Kaspars Grinvalds (Shutterstock)
Whether your health insurance is offered to you by an employer or you get it through the Affordable Care Act marketplace, most plans use the same words to describe exactly what you’re entitled to. Like filing your taxes or fixing a flat tire, health insurance terminology is one of those necessary pieces of knowledge that adults are just expected to have, but if you don’t know what all the lingo means, you’re not alone.
Knowing these words can help you take full advantage of everything your plan entitles you to, which is important, to put it mildly. Let’s look at some terms and why they matter.
The financial health insurance terms you need to know
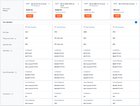
Deductible. Your deductible is the amount you pay for your health services before your health insurance starts paying its share. If your deductible is $1,500, for instance, you have to pay that much on your own before your insurance will kick in and start paying the rest. Some services, like preventive physician visits, might be covered before you pay your deductible, however, so be sure to read all the guidance in your plan. Premium. A premium is what you pay to the insurance company to have your plan. You could pay this monthly—as most people do—or quarterly or annually. If your premium comes straight out of your paycheck, it’s deducted from your pre-tax pay and your employer also likely pays part of the share. If you got your plan through the ACA marketplace, there are tax credits available to help you offset the costs of your premium.Allowed amount. An allowed amount (or eligible expense or payment allowance) is the discounted price your plan has negotiated in advance for the service you’re getting. That means it’s the maximum amount your plan will pay for a covered service.Copay. Your copayment is what you have to pay every time you have a certain service or appointment. These fixed amounts can vary depending on what service you receive. You may owe $50 every time you visit urgent care, for instance, or $20 every time you fill a prescription. Coinsurance. This kicks in after you’ve met your deductible. Coinsurance is the percentage you pay of your medical expenses after you meet it. If your coinsurance rate is 25%, you’ll still pay 25% of your bills after you’ve met your deductible, while your insurance company will pay the other 75%.Out-of-pocket limit. This refers to the maximum you will pay during your policy period, which is typically a year, before your plan starts to pay 100% of your allowed amount. The costs of your deductible, co-pay, and co-insurance are included here, but not your premium. In-network/out-of-network providers. When making appointments with various doctors and service providers, you may notice some are listed as “in-network” while others are “out-of-network.” Any provider or facility that is in-network is one that has contracted with your health insurer to provide services. Depending on your plan, if you visit an out-of-network provider, it may not be covered or might be only partially covered. You can expect a higher deductible and out-of-pocket limit at out-of-network providers. Your coinsurance and copayment may also be higher for out-of-network providers.Preauthorization/prior authorization. A preauthorization is a decision your insurer makes regarding the medical necessity of a service, treatment, drug, or piece of equipment. Also called prior authorization, this is not a guarantee your insurance will cover the cost, but getting one gives you a better shot. Talk to your doctor when you get a prescription and check your insurer’s website to see if it’s covered.
The different kind of insurance plans you need to be familiar with
HMO. This stands for “health maintenance organization” and refers to health plans that are typically lower in cost but offer more limited choice. Under an HMO plan, you usually have to choose an in-network provider (unless you want to pay the whole bill). An HMO typically offers limited or no out-of-network coverage. POS. A point of service plan won’t allow you to get specialized care without a referral from your primary physician. PPO. A preferred provider organization plan is one under which your insurer will pay a portion of your bill, even if you go to a provider outside your network. You don’t even need a referral to do it. Still, try to stay in-network just to save money, if you can. EPO. In an exclusive provider organization plan, you can only use providers, specialists, and facilities that are in the plan’s network (except in cases of emergency). Prescription drug coverage. This refers to health insurance or a plan that helps you pay for your prescription medications. All plans in the ACA cover prescription drugs, but if you get your insurance through your employer, check to be sure yours does. Catastrophic. A catastrophic plan is one that only pays after you’ve reached a very high deductible, but it does so with no copay and no coinsurance. In general, the less expensive your premium is, the higher your deductible is, and catastrophic plans are the best example of that rule. If you pay for one, you won’t be out much money unless something, well, catastrophic happens. Notably, catastrophic plans have to cover your first three primary care visits and certain preventive care visits for free, even if you haven’t met the deductible, which was $7,900 in 2019 and $8,150 in 2020. Generally, to qualify for a catastrophic plan you must be under 30 or be granted a hardship exemption—say, due to the unaffordability of other insurance options.
Why does any of this matter?
Simply put, there are a lot of barriers in the American healthcare system. There aren’t many things you can do about the systemic ones, but what you can do is arm yourself with information about what you’re entitled to.
Dr. Gerald Kominski, senior fellow at the UCLA Center for Health Policy Research, is all about healthcare literacy, and he told Lifehacker why consumers need to know this stuff. Kominski not only studies the barriers to healthcare access in the country, but has experienced them firsthand. He explained that, like many people, he found one of his existing prescriptions wasn’t covered without a prior authorization when he switched to a new insurance provider. His new insurer required him to try other medications and demonstrate that they weren’t working before they would consider covering the one he’d been on for years, but he was “unwilling to experiment.” Instead, he got a GoodRx card, which provides users with coupons for drugs. The coupons can’t be used in conjunction with insurance, but they’re a great option and the service is free.
“The question we often ask is, ‘How many PhDs does it take to figure out your health insurance benefits?’” he said. “Health insurance is so complicated and there are so many things that can vary across policies that there’s a lot of confusion among the general public, much less among people who work in the field. I can’t tell you how many health professionals I’ve dealt with over the years who don’t fully understand the insurance they have—and they work as clinicians.”
Simply put, you’re not alone if you’re confused about what your policy does and does not cover, but it’s imperative you try to figure it all out before an emergency happens.
“It’s really important for consumers to know the specifics of their policies,” Kominski said. “Otherwise, you can find yourself in a situation where suddenly you get a large bill that you weren’t expecting. It may or may not be something that you ultimately have to pay, but this is your best protection to avoid getting a large, unexpected bill, which are also known as ‘surprise bills.’”
If you do get a surprise bill, file a request for review with your insurance company and document the circumstances. Document everything, in fact. Kominski also recommended keeping track of your out-of-pocket expenses and, when you meet your deductible, proactively letting your insurance company know. Some insurers are good about tracking that and notifying plan holders, he said, but others aren’t. Don’t let your insurer’s lack of organization cost you money.